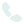
EndoAVF
Percutaneous Fistula Creation - EndoAVF Procedure for Hemodialysis Access
Benefits of Choosing EndoAVF
- Minimally Invasive: EndoAVF is a less invasive procedure compared to traditional surgical fistula creation, resulting in smaller incisions and less trauma to the body.
- Reduced Recovery Time: Patients typically experience faster recovery times and can resume normal activities more quickly.
- Lower Risk of Infection: The minimally invasive nature of EndoAVF reduces the risk of infection compared to open surgical procedures.
- Less Scarring: EndoAVF results in minimal scarring due to the smaller incisions required.
- Outpatient Procedure: Often performed as an outpatient procedure, reducing the need for hospital stays.
- Improved Patient Comfort: Reduced pain and discomfort post-procedure compared to traditional surgery.
- Fewer Complications: Lower risk of complications such as wound infections and hematomas.
- Higher Initial Success Rate: EndoAVF procedures generally have a higher initial success rate in creating functional fistulas.
- Preservation of Vein Integrity: Better preservation of vein structure and integrity, which is important for future access sites.
- Enhanced Cosmetic Outcomes: Improved cosmetic results due to less visible scarring and smaller incision sites.
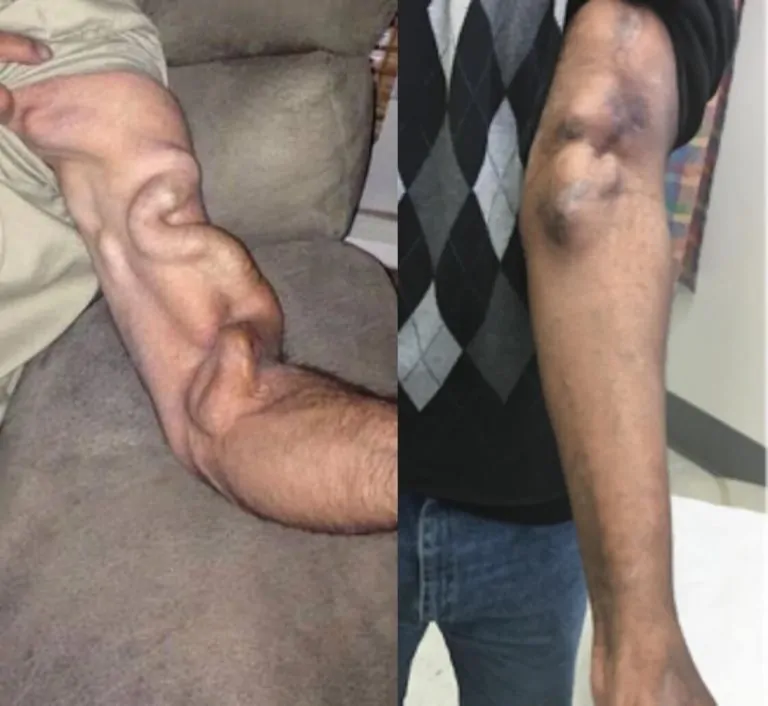
Surgical Fistula Creation
A surgical fistula is the traditional method of creating a dialysis access point. During this procedure, a vascular surgeon makes a small incision in the arm to connect an artery directly to a vein. This connection increases blood flow, helping the vein grow stronger and larger over time so it can support regular dialysis treatments.
Surgical fistulas have been used for decades and are known for their long-term durability and proven success rates. However, because it involves an open incision, recovery may take longer and there can be some visible scarring. For many patients, though, a surgical fistula remains a trusted and effective choice for reliable dialysis access.
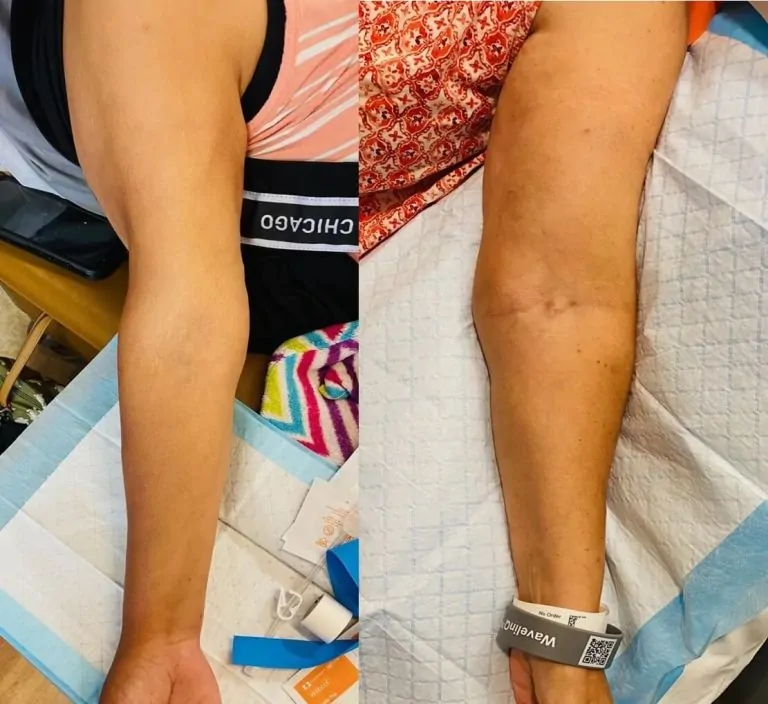
EndoAVF (Endovascular Arteriovenous Fistula) - a Minimally Invasive Procedure
A minimally invasive EndoAVF, or endovascular arteriovenous fistula, offers a modern alternative to traditional surgery. Instead of an incision, this procedure uses a catheter-based technique guided by ultrasound or imaging to create the fistula internally. The connection between the artery and vein is made through a small puncture in the skin. No stitches required.
Because it avoids open surgery, EndoAVF typically allows for:
- Faster recovery times
- Less post-procedure discomfort
- Lower risk of infection
- Little to no visible scarring
EndoAVF provides comparable long-term performance to surgical fistulas while offering a gentler, more comfortable experience for patients seeking minimally invasive dialysis access options.
Ideal Candidates for EndoAVF
EndoAVF is particularly beneficial for patients who:
- Require long-term hemodialysis.
- Are not suitable candidates for traditional surgical AVF creation due to medical reasons.
- Prefer a less invasive option with quicker recovery and fewer complications.
By offering a minimally invasive alternative to surgical fistula creation, EndoAVF provides an effective and patient-friendly solution for establishing reliable hemodialysis access.
Contact Us Today


What to Expect from Your Visit to Pedes
Ultrasound
Advanced ultrasound-guided examination techniques will be used to visualize the veins, arteries, or both, in your legs. This is often used in the diagnostic process to detect the presence and extent of disease.
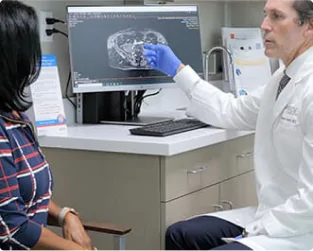
Consult
Once we review the results of your diagnostic tests, our physicians will collaborate with you to develop a personalized treatment plan, ensuring the best course of treatment for your specific condition.
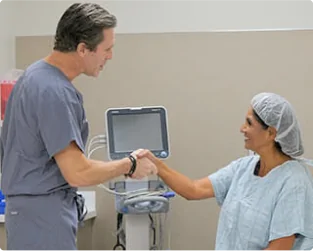
Treatment
Your treatment plan will be personalized to you and your individual needs. At Pedes, we specialize in minimally invasive procedures and nonsurgical treatments, all of which are performed by our dedicated vascular physicians within the comfort of our state-of-the-art facility.

Follow up
We ensure our patients receive continuous care and support with regular follow-up visits. Each follow-up visit is scheduled at the time of your in-office appointment. Should you have a concern between
appointments, we encourage you to call our office and get scheduled at any time.

Treatment Options
Learn more about our treatment options

What to Expect
Learn more about our what to expect

Vascular Disease
Return to the interactive body page