Knee Osteoarthritis (OA)
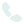
What is Osteoarthritis of the Knee?
Knee osteoarthritis is the most common cause of knee pain. This pain may come and go, become worse over time, or be accompanied by other symptoms like knee stiffness. OA develops due to degeneration of the cartilage, which causes friction between bones and bone tissue changes, leading to pain and limited mobility. Damaged cartilage can also lead to the development of bone spurs, hardened tibia and femur bones, cysts, and bone marrow lesions.
Symptoms of Knee Osteoarthritis
For most people, OA symptoms come and go but worsen over time. While it is easy to dismiss early knee OA signs and symptoms, the symptoms become worse if left untreated, causing mobility issues. Some of the most common signs and symptoms of knee OA include:
Knee Pain
Swelling
Stiffness
Redness and Warmth
Reduced Range of Motion
Worsening Symptoms with Inactivity
Popping or Crunching
Buckling or Locking Up
Causes & Risk Factors of Knee Osteoarthritis
Although knee OA affects as many as 45% of people in their lifetime, the exact cause is unknown. However, researchers have discovered several risks that increase the chances of developing the condition. Risk factors include:
- Advanced age
- Obesity
- Joint trauma or stress
- Family history
- Congenital disabilities or illnesses
- Lack of exercise
- Poor muscle tone
- Being female
photo credit to theii.org
Diagnosing Knee Osteoarthritis
The diagnosis of knee OA involves a comprehensive physical examination by one of our vascular specialists, coupled with a detailed understanding of your medical history and current symptoms. This process may be supplemented with further diagnostic tests such as X-rays and MRI scans to gain an accurate insight into the state of cartilage damage or the presence of bone spurs. Moreover, your doctor may also request blood tests to eliminate the possibility of other conditions causing knee pain.
photo credit to theii.org
Knee Osteoarthritis Treatments
Like most other diseases, addressing the symptoms of knee OA from early stages helps prevent the condition from worsening. Although damage to the joints may not be reversible, our comprehensive treatments aim to prevent future damage. The most common courses of treatment for knee OA include:
Genicular artery embolization is a new and advanced minimally invasive procedure that provides immediate and long-term pain relief for patients suffering from osteoarthritis (OA). The procedure reduces the flow of blood to the lining of the knee. By blocking these arteries, the inflammation that is associated with osteoarthritis reduces significantly, eliminating knee pain.
Learn more about genicular artery embolization.
Lifestyle modifications can help protect your knee health and slow the progression of OA. Our physicians may recommend lifestyle modifications such as minimizing any activities that aggravate the condition, losing weight, and switching to low-impact physical exercise.
The use of medications may be one of the first steps your physician takes in recommending treatment for your knee OA. Our skilled doctors will be happy to work with you to find the medications that best suit your individual needs. Common types of medications recommended for knee OA include:
- Over-the-counter oral pain medications such as aspirin or
- Prescription oral medications such as ibuprofen and
- Topical medications, either over the counter or
Injections are also effective in treating pain caused by knee OA. Some of the joint injections for knee arthritis include:
- Hyaluronic acid (HA) injections, also known as viscosupplementation
- Platelet-rich plasma (PRP) therapy injections
- Stem cell injections
- Prolotherapy, or the use of irritants to boost the body’s natural healing
Physical therapy exercises will help strengthen the knees’ muscles and stretch inflexible, tight muscles such as the hamstring. Physical therapy programs may also include aerobic exercise that encourage proper circulation, and gait and posture training to help eliminate the stress on the knee that may be causing the pain and discomfort.
Knee Osteoarthritis Specialist in Irvine, CA
If you’re feeling pain due to knee osteoarthritis, don’t delay in contacting our vascular specialists today. Give us a call at Pedes Orange County in Irvine, CA, at (949) 387-4724 to schedule an appointment with one of our expert physicians or connect with our supportive staff online to learn more about our specialized knee osteoarthritis treatments. We look forward to helping you live a pain-free life.
Non-Invasive Procedure Performed at Pedes Orange County
Geniculate Artery Embolization (GAE)
Geniculate Artery Embolization (GAE), also known as genicular artery embolization, is a new and advanced minimally invasive procedure that provides immediate and long-term pain relief for patients suffering from osteoarthritis (OA). The procedure reduces the flow of blood to the synovium (the lining of the knee). By blocking these arteries, the inflammation that is associated with osteoarthritis reduces significantly, eliminating knee pain. Is GAE suitable for me? What benefits does it have over traditional OA treatments? Before answering these questions, let us first discuss what osteoarthritis is and its effect on our wellbeing.
Contact Us Today


What to Expect from Your Visit to Pedes
Ultrasound
Advanced ultrasound-guided examination techniques will be used to visualize the veins, arteries, or both, in your legs. This is often used in the diagnostic process to detect the presence and extent of disease.
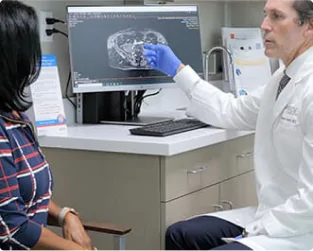
Consult
Once we review the results of your diagnostic tests, our physicians will collaborate with you to develop a personalized treatment plan, ensuring the best course of treatment for your specific condition.
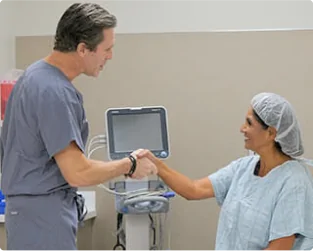
Treatment
Your treatment plan will be personalized to you and your individual needs. At Pedes, we specialize in minimally invasive procedures and nonsurgical treatments, all of which are performed by our dedicated vascular physicians within the comfort of our state-of-the-art facility.

Follow up
We ensure our patients receive continuous care and support with regular follow-up visits. Each follow-up visit is scheduled at the time of your in-office appointment. Should you have a concern between appointments, we encourage you to call our office and get scheduled at any time.
Vascular Disease
Pre-register for your visit to Pedes Orange County by downloading our patient forms.
The physicians at Pedes Orange County devote their lives to saving limbs and minimizing pain. Our conveniently located, state-of-the-art facility is designed for your comfort and utilizes cutting-edge technology to provide minimally invasive treatments. Our vascular specialists are board-certified and some of the best in Southern California. Personable staff members make every visit a positive experience, with short wait times and an efficient, streamlined process that ensures you leave feeling educated and confident that you are in good hands.