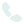
Varicose Veins
What Are Varicose Veins?
Symptoms of Varicose Veins
Varicose veins are twisted, enlarged superficial veins that can cause discomfort and cosmetic concerns. They often present with various symptoms that may affect daily activities and overall well-being.
Common varicose vein symptoms include:
- Aching or heavy sensation in the legs
- Burning, throbbing, or muscle cramping
- Swelling in the lower legs
- Itching around one or more veins
- Skin discoloration around the affected veins
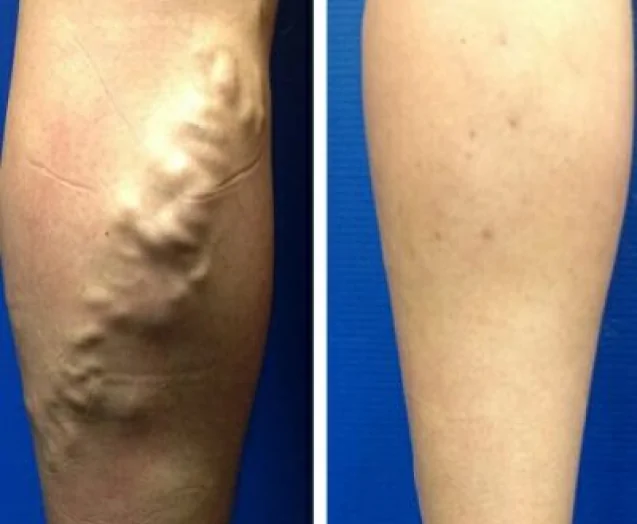
Causes of Varicose Veins
Varicose veins are most commonly caused by valves within the veins malfunctioning. Rather than allowing blood to flow smoothly back to the heart, damaged or worn valves allow the blood to backflow and pool within the veins. This backflow causes the signature swelling and enlargement that we see in varicose veins.
While damaged or missing valves within the veins are the most common cause of varicose veins, other less common causes include:
- Inflammation in the veins (phlebitis).
- Congenital abnormalities within the veins.
- Blood clots or other conditions that may obstruct blood flow to the heart.
Common risk factors associated with the development of varicose veins and other venous diseases include older age, pregnancy, sitting or standing for long periods of time, obesity, and genetic factors.
Varicose Veins Complications
Various studies show that women are more susceptible to varicose veins than men are. Hormonal changes during pregnancy or before the menstrual period cause the veins’ walls to relax, leading to blood backflow. When blood pools in the damaged veins, the blood vessels become painful and swollen, increasing the risk of blood clots.
If you experience chronic inflammation in the veins in your legs, seek medical attention from our vascular doctors immediately. Blood clots that are untreated for prolonged periods may move up the veins and have the potential to cause a stroke. Additionally, hormone treatment such as birth control pills can also increase your susceptibility to this condition.
Diagnosing Varicose Veins
Diagnosing varicose veins is typically simple, as the veins are often visible on the skin’s surface.
However, your diagnostic process may include a physical examination and ultrasound imaging to determine the extent of your condition and to view how the veins are functioning deep within the body. Our dedicated vascular doctors may also ask you to describe your symptoms, including any aching or painful symptoms you may feel in your affected limbs.
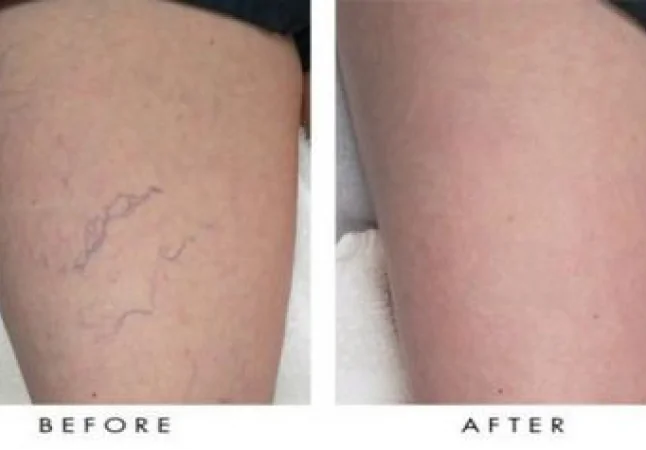
Varicose Vein Treatments in Orange County
- VenaSeal™
- Radiofrequency ablation (FRA)
- Ultrasound-guided sclerotherapy
- Microphlebectomy
Contact Us Today


Our Vascular Disease Physicians
The physicians at Pedes Orange County devote their lives to saving limbs and minimizing pain. Our conveniently located, state-of-the-art facility is designed for your comfort and utilizes cutting-edge technology to provide minimally invasive treatments. Our vascular specialists are board-certified and some of the best in Southern California. Personable staff members make every visit a positive experience, with short wait times and an efficient, streamlined process that ensures you feel educated and confident that you are in good hands.

J. Joseph Hewett, M.D.
Vascular Specialist

Neil K. Goldstein, M.D.
Vascular Specialist

Derrick Tran, MD
Vascular Specialist

Mohammad Jaber, M.D.
Vascular Specialist
Minimally Invasive Spider Vein Treatment
What to Expect from Your Visit to Pedes
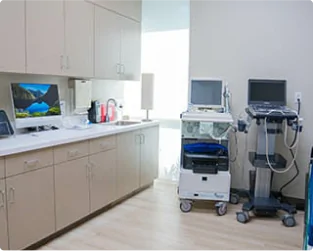
Ultrasound
Advanced ultrasound-guided examination techniques will be used to visualize the veins, arteries, or both, in your legs. This is often used in the diagnostic process to detect the presence and extent of disease.
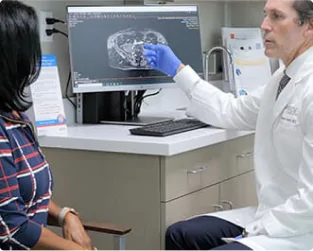
Consult
Once we review the results of your diagnostic tests, our physicians will collaborate with you to develop a personalized treatment plan, ensuring the best course of treatment for your specific condition.
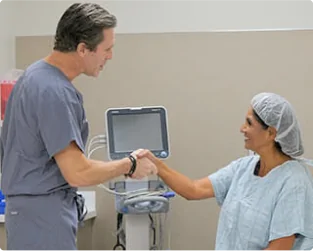
Treatment
Your treatment plan will be personalized to you and your individual needs. At Pedes, we specialize in minimally invasive procedures and nonsurgical treatments, all of which are performed by our dedicated vascular physicians within the comfort of our state-of-the-art facility.